Electrical stimulation therapy has become increasingly accessible for home use, offering drug-free pain management and muscle recovery options. TENS (Transcutaneous Electrical Nerve Stimulation) and EMS (Electrical Muscle Stimulation) devices both deliver electrical impulses through skin electrodes, but they serve fundamentally different purposes and work through distinct physiological mechanisms. Understanding these differences is crucial for choosing the right device for your specific needs. This comprehensive comparison examines both technologies to help you select the most effective solution for pain relief and recovery.
Understanding the Core Technologies
TENS Units: Pain Signal Interruption
TENS units deliver low-voltage electrical current designed to interfere with pain signal transmission to the brain. The technology operates on the gate control theory of pain, which suggests that non-painful input can close the “gates” to painful input, preventing pain sensation from traveling to the central nervous system.
The electrical pulses stimulate sensory nerves at frequencies typically ranging from 2 to 150 Hz. Higher frequencies (80-150 Hz) create a buzzing or tingling sensation that blocks pain signals immediately. Lower frequencies (2-10 Hz) may trigger endorphin release, providing longer-lasting pain relief through the body’s natural pain-relieving chemicals.
TENS therapy is purely sensory—it should not cause visible muscle contractions. The intensity remains below the motor threshold, meaning it affects nerves without triggering muscle movement. Users feel tingling, buzzing, or prickling sensations but shouldn’t see or feel muscles twitching or contracting.
Session duration varies from 15 minutes to several hours depending on pain severity and device settings. Many chronic pain sufferers use TENS throughout the day, while others apply it as needed for acute pain episodes. The treatment is non-invasive and generally considered safe for extended use.
TENS units are FDA-approved for pain management and widely used in physical therapy, sports medicine, and home care. The technology has been refined over decades, with modern devices offering sophisticated programming and user-friendly controls.
EMS Units: Muscle Contraction and Recovery
EMS units deliver electrical impulses designed to cause muscle contractions. The current bypasses the nervous system’s normal pathways and directly stimulates motor nerves, forcing muscles to contract involuntarily. This mimics the body’s natural muscle activation process but without voluntary effort.
The electrical frequency for EMS typically ranges from 1 to 120 Hz, with intensity levels high enough to produce visible and palpable muscle contractions. The sensation feels like forceful muscle squeezing or pumping that you can see and feel but don’t control.
EMS serves multiple purposes: muscle strengthening, injury recovery, muscle re-education after injury or surgery, and reducing muscle atrophy. Athletes use EMS for supplemental training and recovery, while rehabilitation patients use it to maintain muscle function during immobilization or regain strength after injury.
Treatment programs involve repeated contraction-relaxation cycles. A typical session includes 5-10 seconds of contraction followed by rest periods, repeated for 15-30 minutes. The forced contractions fatigue muscles similar to exercise, requiring recovery time between sessions.
EMS has applications beyond recovery—it’s used in physical therapy for muscle re-education, post-surgical rehabilitation, and preventing muscle wasting in bedridden patients. The technology helps maintain muscle mass and function when normal exercise isn’t possible.
Pain Relief Mechanisms and Effectiveness
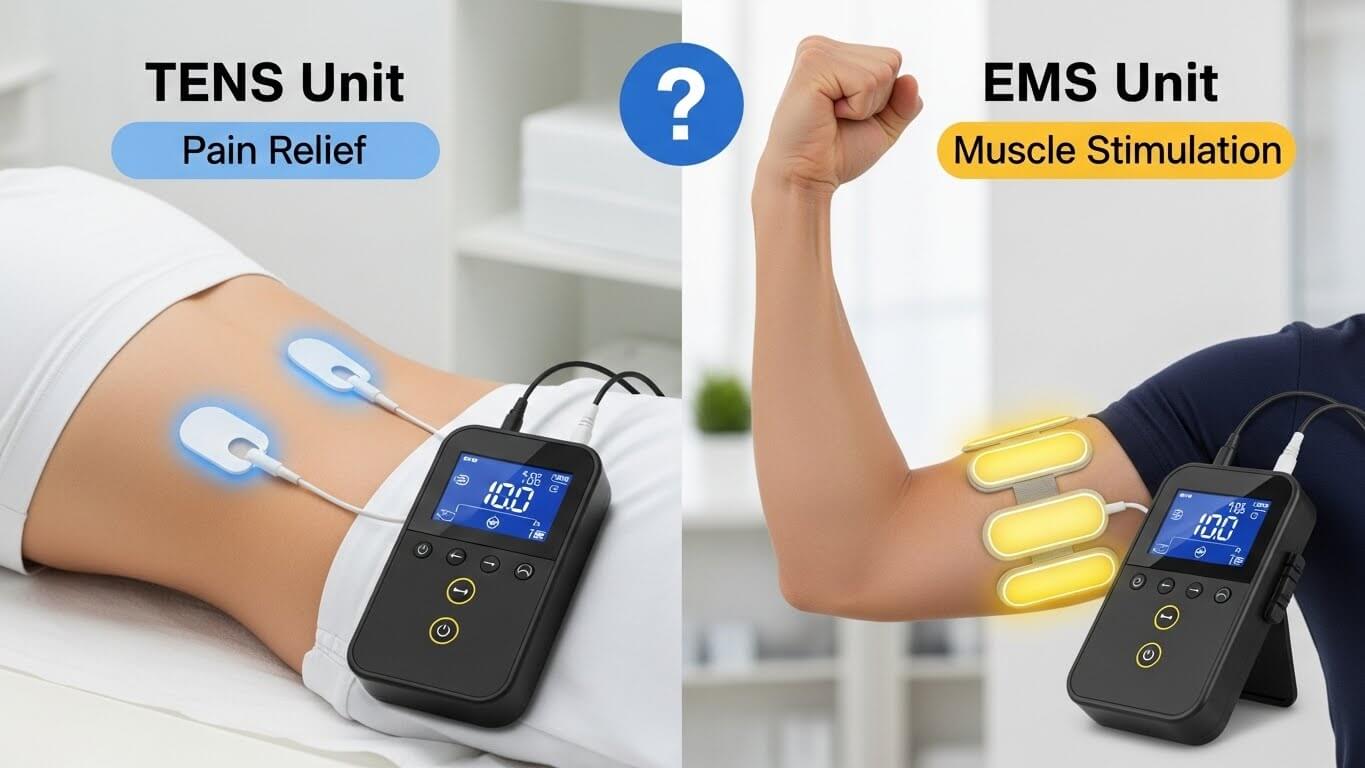
TENS for Pain Management
TENS provides pain relief through two primary mechanisms. High-frequency stimulation (conventional TENS) creates immediate pain relief by overwhelming pain signals—the tingling sensation essentially drowns out pain. This effect begins within minutes but typically ends shortly after removing the electrodes.
Low-frequency stimulation (acupuncture-like TENS) triggers endorphin release, providing pain relief that may last hours after treatment ends. The endorphins act as natural pain relievers, offering benefits beyond the immediate session. However, this effect takes 30-40 minutes to develop fully.
Research on TENS effectiveness shows mixed results depending on condition and application. A 2020 Cochrane review found that TENS can provide short-term pain relief for various conditions but evidence quality varies. The effectiveness seems highly individual; some people experience dramatic relief while others notice minimal benefits.
For acute pain like post-operative discomfort, sports injuries, or labor pain, TENS often provides measurable relief. Studies show reduced pain scores and decreased analgesic medication use when TENS is combined with standard pain management.
Chronic pain response varies significantly. Conditions like osteoarthritis, fibromyalgia, and neuropathic pain show inconsistent results across studies. Some patients report substantial long-term relief, while others find TENS ineffective. The individual variation makes prediction difficult without trial.
TENS works best for well-localized pain where electrodes can be placed accurately around the painful area. Diffuse or deep visceral pain responds less predictably to TENS therapy. The technology excels at addressing superficial musculoskeletal pain.
EMS for Pain Relief
EMS addresses pain indirectly through muscle-related mechanisms rather than direct pain signal interference. The muscle contractions improve circulation, bringing fresh blood and nutrients while removing metabolic waste products. This enhanced circulation can reduce inflammation and accelerate healing, secondarily reducing pain.
Muscle spasms and tension contribute to many pain conditions. EMS can help relax contracted muscles through induced fatigue. After repeated contractions, muscles enter a relaxation phase that may provide relief from tension-related pain.
For pain caused by muscle weakness or imbalance, EMS strengthens targeted muscles, addressing the underlying cause rather than just symptoms. This approach provides more durable pain relief by correcting mechanical issues contributing to discomfort.
Research shows EMS can reduce pain in specific contexts. A 2016 study in the Journal of Strength and Conditioning Research found that EMS reduced DOMS (delayed onset muscle soreness) when applied immediately after exercise. The mechanism appears to be enhanced recovery rather than direct pain interference.
However, EMS is not designed for acute pain relief. During the actual treatment, the forced muscle contractions can be uncomfortable or even increase pain temporarily. The relief comes afterward through improved muscle function and recovery, not during the session itself.
For chronic pain rooted in muscle dysfunction, weakness, or poor circulation, EMS may provide superior long-term benefits compared to TENS. By addressing underlying causes rather than just blocking pain signals, EMS can create lasting improvements.
Target Conditions and Applications
Ideal Conditions for TENS
Back pain, especially chronic lower back pain, represents one of TENS therapy’s most common applications. Electrode placement around the painful area can provide immediate relief for many sufferers. The portable nature allows using TENS while sitting at work or during daily activities.
Arthritis pain in joints like knees, hands, or shoulders responds well to TENS. The localized nature of joint pain allows precise electrode placement for targeted relief. Many arthritis patients use TENS as part of comprehensive pain management to reduce medication dependence.
Neuropathic pain from conditions like diabetic neuropathy or post-herpetic neuralgia may respond to TENS. The electrical stimulation can interrupt the abnormal nerve signaling causing pain, though results vary widely among individuals.
Menstrual cramps and labor pain have shown positive response to TENS in clinical studies. The non-pharmaceutical nature makes TENS attractive during pregnancy and for people avoiding pain medications. Many hospitals offer TENS units for labor pain management.
Sports injuries creating acute pain benefit from TENS during the healing process. The ability to reduce pain without medications that might mask further injury makes TENS valuable for athletes wanting to monitor their recovery accurately.
Headaches and migraines show variable response to TENS. Some sufferers find relief with electrodes placed on the neck, temples, or forehead, while others experience no benefit. The accessibility and safety make it worth trying despite inconsistent research results.
Ideal Conditions for EMS
Muscle atrophy prevention during immobilization uses EMS to maintain muscle mass and function. When injuries require limb immobilization or bed rest, EMS helps prevent the rapid muscle loss that normally occurs. This application is well-established in rehabilitation medicine.
Post-surgical recovery, particularly after orthopedic procedures, benefits from EMS to rebuild strength. The technology helps patients regain muscle function faster than exercise alone during early rehabilitation when full weight-bearing or movement isn’t possible.
Athletic recovery and training supplementation represents a growing EMS application. Athletes use EMS to enhance recovery between workouts, supplement training volume safely, and target specific muscle groups for development.
Muscle imbalances contributing to chronic pain respond well to EMS strengthening. When weakness in one muscle group causes compensatory pain in others, selectively strengthening the weak muscles through EMS can resolve the underlying dysfunction.
Circulation-related conditions like some peripheral vascular disease cases benefit from EMS-induced muscle pumping action. The contractions help move blood through extremities, potentially reducing symptoms related to poor circulation.
Muscle spasm and chronic tension sometimes respond to EMS-induced fatigue and subsequent relaxation. While the mechanism seems counterintuitive, fatiguing spasmed muscles can help them relax more completely afterward.
Ease of Use and Learning Curve
TENS Unit Operation
TENS units are generally user-friendly with straightforward controls. Most devices include preset programs for different pain types—acute, chronic, arthritis, back pain—that automatically set appropriate frequency, intensity, and pulse width. Users simply select the program and adjust intensity to comfort level.
Electrode placement is crucial but relatively intuitive. Place pads around the painful area, typically flanking the pain site or along nerve pathways. Most TENS units include placement guides with diagrams for common conditions. Some trial and error may be needed to find optimal placement.
Intensity adjustment is simple—increase until you feel strong tingling without discomfort or muscle contractions. If muscles start twitching, the intensity is too high for TENS therapy. The sensation should be pronounced but comfortable.
Session management requires minimal attention. Set the timer, apply the device, and continue normal (non-vigorous) activities. Most people can use TENS while working, watching TV, or resting. The passive nature makes it easy to incorporate into daily routines.
Common mistakes include insufficient intensity (too subtle to be effective), electrode placement too far from pain site, and expecting instant relief with low-frequency settings that take time to trigger endorphin release. These issues are easily corrected with basic understanding.
EMS Unit Complexity
EMS units are more complex due to muscle-specific programming requirements. Different muscles and goals require different frequencies, pulse widths, and contraction patterns. While preset programs exist, optimal results often require customization.
Electrode placement demands more precision than TENS. Pads must be positioned over motor points—specific locations where nerves enter muscles—for effective contractions. Improper placement causes weak, inefficient contractions or uncomfortable sensations without proper muscle engagement.
Intensity must be high enough to produce strong, visible contractions but not so high as to cause cramping or pain. Finding this balance takes practice and varies by muscle group, fatigue level, and individual tolerance. The learning curve is steeper than TENS.
Sessions require monitoring and adjustment. As muscles fatigue during the session, you may need to increase intensity to maintain contraction strength. Unlike TENS, you can’t simply set and forget—active management optimizes results.
Most users require several sessions to master effective EMS use. Understanding contraction patterns, rest intervals, and progression takes time. Professional guidance from physical therapists or trainers accelerates the learning process but isn’t always accessible.
Safety Considerations and Contraindications
TENS Safety Profile
TENS is considered very safe when used as directed. The low-voltage current cannot cause tissue damage or serious adverse effects in most users. The primary risks are minor skin irritation from electrodes and potential skin burns if using damaged equipment.
Contraindications include pacemakers or other implanted electrical devices, as TENS interference could affect device function. Pregnancy requires caution—avoid electrode placement on the abdomen, but TENS is often safe for back pain and approved for labor pain.
People should not use TENS over the carotid sinus (neck area near the carotid artery), across the chest near the heart, or on the front of the neck, as stimulation in these areas could cause adverse reactions. Avoid placement directly over the spine, on broken skin, or over areas with reduced sensation.
Cancer patients should consult oncologists before using TENS, particularly avoiding placement over tumors. Epilepsy patients should use caution and medical supervision, as electrical stimulation could theoretically trigger seizures, though this is rare.
Skin reactions from electrode gel or adhesive affect some users. Rotating electrode placement slightly, using hypoallergenic electrodes, or applying protective skin prep can minimize irritation. These reactions are inconvenient but not dangerous.
EMS Safety Concerns
EMS shares TENS contraindications regarding pacemakers, pregnancy (on abdomen), and electrical implants. The higher intensity of EMS makes these contraindications more critical—strictly avoid use in these situations.
The forced muscle contractions can cause muscle soreness, cramping, or even strain if intensity is excessive or rest periods insufficient. Unlike voluntary exercise where fatigue signals limit exertion, EMS can push muscles beyond safe limits if misused.
Joint stress from strong muscle contractions without appropriate stabilization could theoretically cause injury. When using EMS on muscles that cross joints, ensure joints are properly supported to prevent abnormal forces.
People with muscle or nerve disorders should consult physicians before using EMS. Conditions affecting muscle function or nerve signaling may respond unpredictably to electrical stimulation.
Overuse represents a genuine concern with EMS. Some users, seeing muscle contractions as “free exercise,” apply EMS daily or multiple times daily. Muscles need recovery time from EMS just like regular exercise. Overuse can lead to fatigue, performance decrements, and injury.
Cost and Accessibility
TENS Unit Investment
TENS units range from $20 to $200 for consumer models. Budget devices at $20-$40 provide basic functionality adequate for occasional use. Mid-range units ($50-$100) offer better build quality, more programs, and dual-channel output for treating two areas simultaneously.
Professional-grade TENS units cost $150-$300 but offer superior electrode quality, battery life, and sophisticated programming. These devices last longer and provide more consistent performance than budget alternatives.
Replacement electrodes represent the primary ongoing cost. Quality reusable electrodes cost $10-$20 for a set of four and last 20-30 applications with proper care. Cheaper electrodes may need replacement every 10-15 uses. Annual electrode costs typically run $30-$60 with regular use.
Insurance coverage varies. Some plans cover TENS units for chronic pain with physician prescription. Medicare covers TENS for specific conditions after a 30-day trial demonstrates effectiveness. Check coverage before purchasing—medical-grade units bought through healthcare providers may be covered while consumer devices aren’t.
EMS Unit Pricing
Consumer EMS devices range from $30 to $300. Budget units ($30-$80) provide basic muscle stimulation adequate for recovery and general use. Mid-range models ($100-$200) offer better programming, higher power output, and multiple channels.
Professional EMS systems used by physical therapists and athletic trainers cost $400-$1,500+. These devices deliver superior power, precision, and programming compared to consumer models. They’re designed for clinical use with higher duty cycles and more sophisticated controls.
Replacement electrodes are identical to TENS electrodes, so costs are comparable. High-quality electrodes are essential for effective EMS since strong contractions require excellent electrode-skin contact.
Insurance rarely covers EMS devices for home use, considering them exercise equipment rather than medical devices. Professional EMS therapy in clinical settings may be covered, but take-home units typically aren’t.
Combination Devices and Hybrid Options
TENS/EMS Combo Units
Many modern devices combine both TENS and EMS functionality in a single unit. These combination devices offer versatility, allowing users to choose appropriate therapy based on current needs. Price points range from $40 to $200, providing good value compared to buying separate devices.
The dual functionality makes sense for athletes and active individuals who might use TENS for pain relief and EMS for recovery and strengthening. Having one device that addresses multiple needs simplifies equipment management and reduces total cost.
However, combination devices sometimes compromise on specialization. Dedicated TENS or EMS units may offer superior programming and performance for their specific function compared to combination units at similar price points.
Quality varies significantly in combination devices. Premium combinations from established brands perform well for both functions. Budget combinations may excel at one function while delivering mediocre performance in the other.
When Combination Devices Make Sense
Athletes managing both pain and recovery needs benefit from combination devices. Use TENS after workouts for immediate pain relief, then switch to EMS for recovery and strengthening. This comprehensive approach addresses multiple recovery aspects with one device.
People uncertain about their needs appreciate the flexibility to try both therapies. A combination device allows experimenting with TENS and EMS to determine which provides better results before investing in specialized equipment.
Budget constraints make combinations attractive. Spending $80 on a quality combination device provides both therapies for less than purchasing separate specialized units.
Making Your Decision
Choose TENS If:
Your primary goal is pain relief rather than muscle strengthening or recovery. TENS directly addresses pain through nerve stimulation, making it the appropriate choice for pain management.
You experience chronic pain from conditions like arthritis, neuropathy, or chronic back pain. The ability to use TENS throughout the day for ongoing relief suits chronic pain management better than EMS.
You want a simple, set-and-forget device requiring minimal learning curve. TENS is easier to use effectively with less technique-dependent results than EMS.
You need pain relief during activities rather than just during rest. TENS allows continuing work, light activities, or daily tasks while receiving treatment.
Budget is extremely limited and you need the most economical option. Basic TENS units cost less and require less sophisticated programming than effective EMS devices.
Choose EMS If:
Muscle weakness, atrophy, or dysfunction contributes to your discomfort. EMS addresses underlying muscular causes rather than just pain symptoms.
You’re recovering from injury or surgery requiring muscle rehabilitation. EMS helps rebuild strength and function during recovery periods.
Athletic recovery and supplemental training interest you. EMS provides recovery benefits and training supplementation beyond what TENS offers.
You’re willing to invest time learning proper technique and electrode placement. EMS requires more sophisticated use but provides benefits beyond pain relief.
Circulation improvement or muscle spasm reduction through contraction-relaxation cycles would benefit your condition.
Consider Combination Devices If:
You experience both acute pain and muscle dysfunction. Having both therapies available allows addressing different aspects of recovery.
You’re an athlete needing both pain management and recovery tools. The versatility supports comprehensive recovery strategies.
Budget allows for quality combination units but not separate specialized devices. Good combinations provide adequate performance in both functions for less than buying two separate units.
You want to try both therapies before committing to specialized equipment. Combinations allow experimentation to determine which therapy suits your needs better.
Frequently Asked Questions
Can I use TENS and EMS at the same time on different body parts?
Yes, using separate devices on different areas simultaneously is safe. Some athletes use TENS on a painful area while applying EMS to another muscle group for recovery. However, don’t apply both TENS and EMS to the same area simultaneously—the different purposes and settings conflict. Use them sequentially instead, perhaps TENS first for pain relief, then EMS for strengthening or recovery.
How long does pain relief last after a TENS session?
High-frequency TENS provides pain relief during and shortly after treatment, typically 15-30 minutes after removing electrodes. Low-frequency TENS triggering endorphin release may provide relief lasting several hours. Regular use sometimes creates cumulative benefits where pain relief extends longer over time. Individual response varies significantly—some people experience hours of relief while others notice benefit only during active treatment.
Can EMS build muscle as effectively as regular exercise?
EMS cannot replace regular exercise for overall fitness and strength development. Research shows EMS can increase muscle strength and size, but gains are generally smaller than from voluntary exercise. EMS works best as a supplement to traditional training or during rehabilitation when normal exercise isn’t possible. Elite athletes use EMS to add training volume without additional joint stress or to target specific muscles difficult to isolate through conventional exercise.
Why do some professional athletes use both TENS and EMS?
Professional athletes often face both pain management needs and recovery/strengthening demands. TENS addresses acute pain from training or competition without medications that might affect performance or violate regulations. EMS accelerates recovery between sessions and helps maintain muscle function during injury rehabilitation. The combination provides comprehensive support for the demanding physical requirements of professional sports.
Are there any medications that interact with TENS or EMS?
Neither TENS nor EMS has significant drug interactions in the traditional sense. However, pain medications might mask the sensations needed to properly adjust device intensity, potentially leading to overuse or skin irritation. Muscle relaxants might affect EMS effectiveness by reducing muscle response to stimulation. Always inform healthcare providers about electrical stimulation use when discussing treatment plans.
How often can I safely use TENS or EMS?
TENS can be used throughout the day as needed for pain relief, with some chronic pain patients using it for hours daily. There are no strict usage limits for TENS beyond skin irritation prevention—rotate electrode placement slightly and give skin breaks. EMS should be limited like regular exercise—allow 24-48 hours between sessions on the same muscle group for recovery. Using EMS daily on different muscle groups is acceptable, but don’t overstimulate the same muscles without recovery time.
Will insurance cover TENS or EMS devices?
Insurance coverage for TENS is possible with physician prescription for approved indications like chronic pain. Medicare covers TENS for chronic low back pain after a supervised 30-day trial proves effective. Coverage varies by insurer and specific condition. EMS is rarely covered for home use, as insurance typically classifies it as exercise equipment rather than medical therapy. Professional therapy sessions using these devices may be covered when prescribed as part of rehabilitation.
Can TENS or EMS cause muscle damage or nerve damage?
When used properly, both devices are very safe and won’t cause muscle or nerve damage. The electrical current is too low to damage tissues. However, misuse can cause problems—excessive EMS intensity or duration can create severe muscle soreness or strain similar to overtraining. Damaged equipment or improper electrode contact could theoretically cause skin burns. Using devices as directed with FDA-cleared products poses minimal risk.
Conclusion
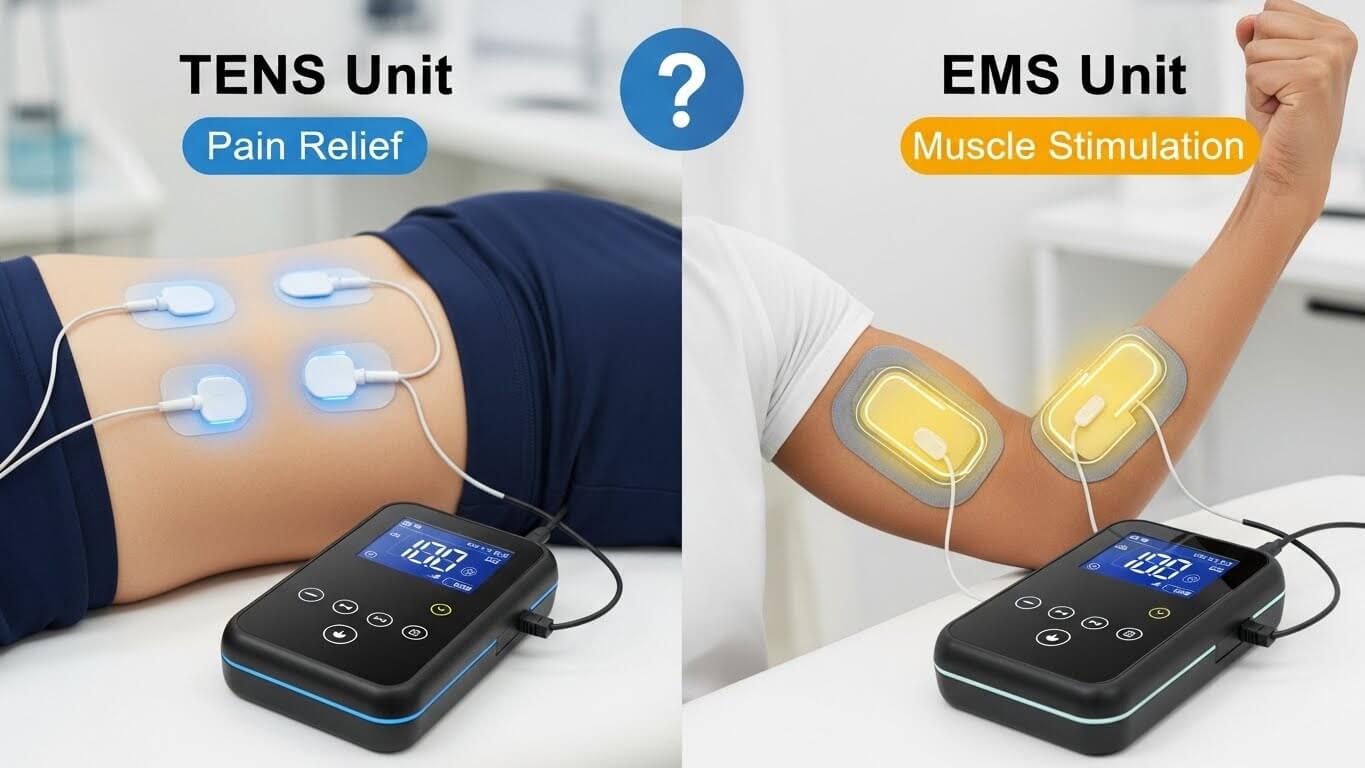
TENS and EMS serve fundamentally different purposes despite both using electrical stimulation. TENS excels at pain relief through nerve signal interference and endorphin release, making it the appropriate choice for managing chronic pain, arthritis, sports injuries, and various pain conditions. The ease of use, safety profile, and ability to provide relief during daily activities make TENS valuable for anyone seeking drug-free pain management.
EMS addresses muscular causes of discomfort through forced contractions that strengthen muscles, improve circulation, and enhance recovery. It’s ideal for rehabilitation, preventing muscle atrophy, athletic recovery, and addressing pain rooted in muscle weakness or dysfunction. The learning curve is steeper and results take longer to manifest, but EMS can provide lasting improvements by addressing underlying causes.
For pure pain relief, TENS is the clear winner. It directly targets pain mechanisms and provides faster, more predictable relief for most pain conditions. EMS may eventually reduce pain by improving muscle function, but the relief is secondary to muscular changes rather than immediate pain signal interference.
Many people ultimately benefit from both technologies used strategically. TENS for immediate pain management and EMS for recovery and strengthening creates a comprehensive approach to musculoskeletal health. Combination devices offer good value for those wanting both capabilities without purchasing separate equipment.
Consider your primary goal when choosing. If pain relief is paramount and muscle function isn’t compromised, TENS is the appropriate choice. If muscle weakness, poor recovery, or dysfunction contributes to your discomfort, EMS may provide superior long-term benefits. Budget-conscious users can start with TENS units due to lower costs and simpler operation, adding EMS later if muscle-specific needs emerge.
Both technologies are well-established with decades of clinical use and research support. Neither is a miracle cure, but both provide legitimate therapeutic benefits when applied appropriately. Success depends on matching the technology to your specific condition, using devices correctly, and maintaining realistic expectations about what electrical stimulation can accomplish.
